
DASH Diet vs Mediterranean Diet: Is One a Better Choice?
Inside: I’m often asked about a DASH diet vs Mediterranean diet. Is one better? Research shows each offers benefits, so consider your priorities… and realize it may not be an either-or choice.

Deciding which kind of dog is “best” for you is complex… just like the question of which kind of diet is a better choice.
Which one? When my family and I decided to get a dog, we heard lots of advice about which kind of dog is the “best dog”.
We heard lots of “either-or” choices. Would it be better to have a purebred dog or a mutt? A big dog or a small one? Do you want one that doesn’t bark much, or one that will bark to guard and warn you?
While we each may have our personal favorites, the question really has to be considered in the context of what is “best” for each individual or family.
In the same way, dietitians like me are often asked to help people choose “the best diet”. Giving advice that’s based on the strongest available scientific research, it’s still not a simple question. When it comes to heart health and lower cancer risk, two approaches to eating habits that often come up are the Mediterranean diet and the DASH diet.
KEY TAKE-AWAY POINTS
♦ Research links scores representing a more Mediterranean-style diet with cardiovascular health, although the many variations in this dietary pattern make research complicated.
♦ A Mediterranean-style diet includes an abundance of nutrient-rich plant foods, with fat coming primarily from olive oil, nuts, and other unsaturated fats.
♦ DASH diet research, whether in controlled trials in which a DASH diet is studied as a specific dietary pattern, or in large population studies using a score to identify eating habits most consistent with that pattern, shows a DASH diet is a powerful tool for reducing blood pressure and promoting overall cardiovascular health.
♦ A DASH diet is rich in whole plant foods and limits sodium, saturated fat, and added sugars.
♦ Think options! A DASH diet and a Mediterranean diet are both plant-based diets, but not necessarily plant-only diets. Both are consistent with recommendations to reduce cancer risk, and they can be adapted in multiple ways to meet individual dietary preferences, health concerns, and food preferences.
Why Recommend a Mediterranean Diet? The Evidence

- A meta-analysis of 27 prospective cohort studies found that each additional increase in Mediterranean diet score was associated with a further decrease in cardiovascular disease incidence or mortality.
- An umbrella review of multiple prospective cohort meta-analyses links a more Mediterranean-style diet with lower incidence of heart disease, stroke, and diabetes.
- Highest Mediterranean diet scores compared to lowest scores are associated with lower overall cancer incidence in some analyses of prospective cohort studies, but not in all. Among cancer types, evidence is strongest supporting links to lower risk of colorectal cancer.
- Among people with existing coronary heart disease (CHD), greater adherence to a Mediterranean diet was associated with lower hazard of both recurrent coronary heart disease events and all‐cause mortality.
Evidence on the Mediterranean diet and health began with observations in these populations. Now analyses pulling together results of multiple randomized controlled clinical trials comparing a Mediterranean-style diet to some other diet shows specific effects that are likely contributing to better health.
Systolic Blood Pressure: reduced 0.67 mm Hg [Quality of evidence grade: suggestive]
Diastolic Blood Pressure: reduced 0.94 mm Hg [Quality of evidence grade: suggestive]
LDL Cholesterol: reduced 4.25 mg/dL — but not statistically significant
Blood Triglycerides: reduced 2.71 mg/dL [Quality of evidence grade: weak]
A1C (a measure of blood sugar control over the past 3 months): reduced 0.30
Insulin resistance (HOMA-IR test): reduced 0.45
Metabolic Syndrome 20% decreased risk (and increase in reversal of metabolic syndrome among people who had it also reported) [Quality of evidence grade: weak]
Inflammation measured by hsCRP: reduced 0.98 mg/l [Quality of evidence grade: weak]
Blood vessel health (Endothelial function measured by flow-mediated dilation): improved 1.86% [Quality of evidence grade: weak]
Weight: reduced 3.9 pounds, often analyzed as Body Mass Index (BMI), reduced 0.57 units (kg/m2)
Waist size: reduced just under ¼ inch
**Limited strength of evidence can reflect low statistical power of some studies (for example, related to study design, number of subjects, precision, and variability among individuals).
The Mediterranean Diet: What Are the Fundamentals?

Overall:
- The Mediterranean diet is a plant-focused diet. Emphasis is on vegetables, fruits, whole grains and pulses (like dried beans & lentils)
- Total fat content is not low, but can range between 30% of calories (moderate) and 40% (high). It’s low enough in saturated fat to meet general health recommendations (<10%) — although some specific modifications may be needed to bring levels low enough to meet major recommendations for people with existing cardiovascular disease or elevated LDL or non-HDL cholesterol.
- Most of the fat provided is unsaturated fat.
- Olive oil is the primary source of fat in the traditional Mediterranean diet. This makes the diet high in monounsaturated fat (MUFA). And if Extra Virgin is chosen, olive oil polyphenols and other plant compounds may bring extra protective benefits.
- Nuts are also important. They provide unsaturated fat and potentially protective phytochemicals.
- Fish is included at least two or three times each week. It is eaten more frequently than red meat (which is consumed only monthly or occasionally).
To study long-term health, observational cohort studies use scoring systems to identify how dietary patterns are associated with health.
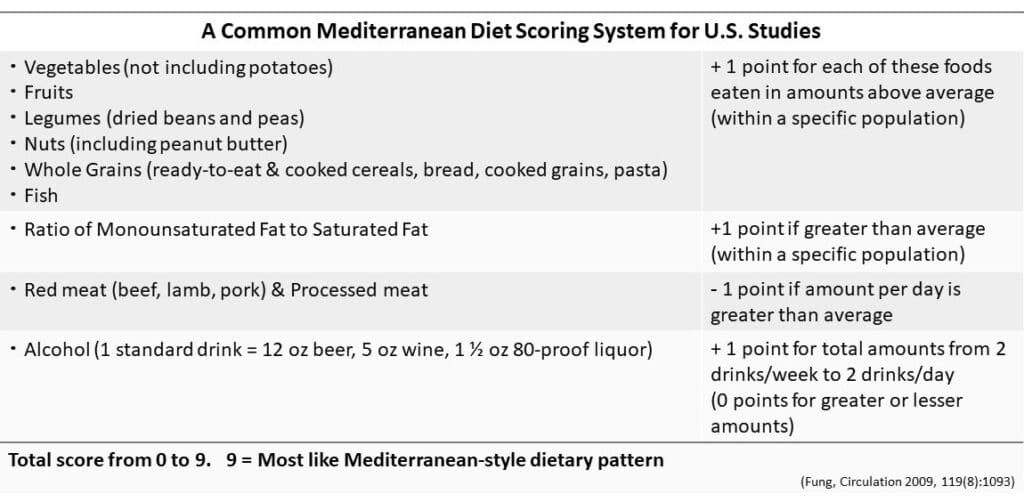
Here’s an example of one of the most common Mediterranean diet scoring systems in US-based studies:
In this scoring system, a point is awarded for higher intake of monounsaturated fat (as would come with more olive oil) in proportion to saturated fat (which could come from butter, meat, and dairy products).
Scoring systems differ: Some score for olive oil or MUFA amounts (instead of the ratio to saturated fat). Some don’t include points for alcohol, since there can be negative health consequences, especially related to cancer risk. Some include a point for limiting sweets or keeping dairy products to moderate use only.
Risk of disease and levels of risk factors may be more strongly tied to a Mediterranean diet score in Mediterranean populations. The same score in a Mediterranean country often represents a diet that’s “more” Mediterranean than a more Mediterranean-style diet in the U.S.
The consistent dietary pattern that Mediterranean diet scores represent is a plant-forward pattern that emphasizes olive oil, nuts, and other unsaturated fats. Share on X
What’s Easily Overlooked About a Mediterranean Diet 
-
- Percent carbohydrate or fat does not define a Mediterranean diet.
- It’s not a vegetarian diet. A Mediterranean diet can be adapted to omit categories of animal foods as desired, but the scores used in research on associations with health allow for modest consumption of meat, poultry, fish and dairy.
- Flavor profile does not define a Mediterranean diet in health research, since it’s not part of Mediterranean diet scores. So people who prefer food with flavor profiles from other areas of the world can still eat a Mediterranean diet.
- What about sodium? No element of Mediterranean diet scores addresses sodium content other than by limiting processed meat. For more influence on blood pressure, pick up the culinary traditions of abundant use of garlic, vinegar, lemon juice, herbs and spices can help keep food flavorful without lots of salt at the table or in highly processed foods.
- What about dairy products? Some studies refer to Mediterranean diets as limiting dairy products, and others refer to types of dairy products chosen (favoring fermented dairy choices of yogurt and cheese). Analysis of which elements of a Mediterranean dietary score are most strongly associated with reduced health risks don’t provide a consistent picture about dairy products. Since growing evidence suggests moderate consumption of dairy products may be linked with lower levels of cardiovascular risk factors and lower risk of Type 2 diabetes, individual factors can be considered to suggest keeping dairy to the Mediterranean tradition of 1-2 servings per day, or allowing for slightly more.
- What about red wine? Moderate amounts (1 to 2 small glasses per day) are intertwined in Mediterranean cultural and culinary traditions. Analyses of dietary score components’ contribution to health outcomes generally suggest that cardiovascular benefits are linked with moderate compared to either excess or avoidance of alcohol; other analyses suggest it is not essential to the diet’s relationship to health. Questions arise because the association of alcohol with increased risk of several cancers and overall chronic disease burden applies equally to wine as to other forms of alcohol. That’s why some adapted Mediterranean diet scores don’t include alcohol. Most researchers and proponents of a Mediterranean diet still consider moderate consumption of wine with meals a component of the diet, although consumption of alcohol is not encouraged for individuals who do not drink.
- Compared to what? Studies that show a Mediterranean diet to be a healthier dietary pattern often compare it to a typical American diet or to a low-fat diet that does not set guidelines for choosing nutrient-rich foods to replace high-fat foods. These studies don’t mean a Mediterranean diet is necessarily more healthful than another plant-forward healthy eating pattern.
◊ ◊ ◊ ◊ ◊ ◊ ◊
Want help figuring out a Mediterranean diet?
For a free guide with 5 doable steps, Click Here.
◊ ◊ ◊ ◊ ◊ ◊ ◊
Why Recommend a DASH Diet? The Evidence

The study focus was specific: Besides reducing sodium, how else could a diet improve blood pressure?
These were the groundbreaking results of one of the earliest DASH diet studies:
- Combining components that create a DASH diet + a reduction in sodium decreased blood pressure more effectively than either DASH diet alone or sodium reduction alone.
- At any level of sodium intake, choosing foods to create a DASH-style pattern can reduce systolic blood pressure. DASH-style eating produces the biggest drops in blood pressure in people with highest sodium consumption.
- Great news for people who have trouble reducing sodium: Incorporating DASH-style food choices can reduce blood pressure as much as a stricter sodium limit in an otherwise unhealthy eating pattern.
To look at long term effects on health, large prospective population studies use scoring systems to represent how people’s diets align with the components of the DASH diet.
- A meta-analysis of 15 prospective cohort studies found that diets most consistent with a DASH diet are associated with 18% fewer deaths from all causes during 10 to 24 years of follow-up compared to diets least like a DASH diet.
- Meta-analyses of multiple prospective cohort studies link a diet more consistent with the DASH diet with lower incidence of cardiovascular disease and diabetes.
- Highest DASH diet scores compared to lowest scores are associated with lower overall cancer incidence or mortality in some analyses of prospective cohort studies, but not in all. Among cancer types, evidence is strongest supporting links to lower risk of colorectal cancer.
- Among people with existing cancer, greater adherence to a DASH diet was associated with lower hazard of both cancer mortality and all‐cause mortality.
Closeup on the DASH Diet (Original Version)
As created for these early studies, the DASH diet is:
- Low in total and saturated fat: Although not as low as some diets (such as Pritikin or Ornish diets), the DASH diet is low in total fat (27% of calories) and saturated fat (6% of calories). It’s categorized as moderate in carbohydrate (55%) and moderate in protein (18%).
- High in fiber, potassium, magnesium, and calcium, with limited added sugars.
- We now know that the emphasis on vegetables, fruits, and whole grains also makes the DASH diet high in a wide range of plant compounds that seem to promote healthy blood vessels. (Check here for my research review on how diet can influence endothelial function and other aspects of vascular health.)
The original trials tested a DASH diet at several different sodium levels. Moving forward, DASH diet trials have limited sodium to no more than 2400 mg a day, unless otherwise specified.
DASH Diet Studies: The Promise Seen in Clinical Trial Research
The DASH diet has been widely studied since those original studies, including more randomized controlled trials. Analyses combining trials shows specific health benefits.
Systolic Blood Pressure: reduced 5.2 mm Hg, a clinically meaningful reduction [Certainty of evidence grade: high or moderate]
Diastolic Blood Pressure: reduced 2.6 mm Hg
- Among people who had high blood pressure in the analysis above, DASH diets decreased blood pressure about 11/6 points, or about double the drop in people who didn’t have high blood pressure.
- A DASH diet reduced blood pressure more than low-sodium diets that did not include DASH food choices. And a DASH diet lowered blood pressure by an additional 3.91/1.56 mm Hg compared to a Mediterranean diet, according to another analysis of randomized controlled trials involving people with elevated blood pressure.
LDL Cholesterol: reduced 3.87 mg/dl [Certainty of evidence grade: moderate]
Blood Triglycerides: reduced 0.00 mg/dl [Certainty of evidence grade: low]
A1C (a measure of blood sugar control over the past 3 months): reduced 0.53 [Certainty of evidence grade: low]
Insulin resistance (HOMA-IR test): reduced 0.05, not statistically significant [Certainty of evidence grade: moderate]
Metabolic Syndrome: limited research; an analysis of cross-sectional studies found 48% decreased risk [Quality of evidence: weak]
Inflammation measured by hsCRP: reduced 0.74 mg/L in trials lasting at least 8 weeks [Certainty of evidence grade: low]
- Among trials comparing a DASH diet to a usual/unhealthy diet, CRP levels decreased 1.01 mg/L; but the decrease was smaller and not statistically significant in comparisons with other healthy diets.
Subclinical heart muscle damage and strain (measured by high-sensitivity cardiac troponin I and N-terminal pro–B-type natriuretic peptide, respectively) were decreased by a DASH diet, according to recent analyses of the original DASH study.
Blood vessel health (Endothelial function measured by flow-mediated dilation): improved 2.5% compared to routine care in adolescents with elevated blood pressure or hypertension in one study.
Weight: reduced 3.1 pounds (statistically significant, but may not be clinically meaningful); often analyzed as Body Mass Index (BMI), reduced 0.42 units (kg/m2)
Waist size: reduced just under ½ inch
**Limited strength of evidence can reflect low statistical power of some studies (for example, from study design, number of subjects, precision, and variability among individuals).
How Effective is a DASH Diet for Weight Loss?
DASH trials intentionally kept weight constant, to test the effect of diet alone on blood pressure.
A DASH diet, with its emphasis on foods that aren’t high in calories, can help weight loss. But especially if portions are excessive, it doesn’t necessarily lead to weight loss.
Yet we know that for many people, having overweight or obesity significantly increases blood pressure. And even modest weight loss can powerfully help reduce high blood pressure.
The ENCORE trial involved people with overweight or obesity who had elevated blood pressure and were not taking any anti-hypertensive medications. After four months:
- A DASH diet only group was asked not to exercise or try to lose weight. They focused on what they ate, with weekly group sessions with a registered dietitian to help overcome barriers of adopting new eating habits.
- This group lost an average of 1 pound. Blood pressure dropped by 11.2 / 7.5 mm Hg.
- A DASH diet plus weight loss group was guided to also reduce calories by about 500 per day and increase physical activity with supervised exercise sessions three times a week.
- This group lost an average of 19 pounds. Blood pressure dropped by 16.1 / 9.9 mm Hg.13 — achieving a blood pressure reduction equivalent to what can be reached with starting dose anti-hypertension medications.
- The combination of a DASH diet, weight loss and physical activity also improved aerobic fitness with exercise capacity increased 19% from baseline, reduced LDL cholesterol by 16 mg/dL from baseline, reduced serum triglycerides by 40 mg/dl from baseline. The combination approach reduced artery stiffness and improved insulin sensitivity and fasting insulin levels even more than the DASH diet alone.
Can You Make a DASH Diet Even Better? OmniHeart!
As positive as the DASH outcomes were, can we tweak the diet to bring even better results?
The OmniHeart trial was designed to answer that question. In this trial, each subject had six weeks on each diet, which is plenty of time to see changes in blood pressure.
- As in the DASH diet studies, none of the OmniHeart participants were taking blood pressure medications and none had diabetes. Initial blood pressure ranged from 120 to 159 / 80 to 99. Based on how blood pressure is categorized today, that means blood pressures ranged from mild elevations to Stage 2 hypertension.
- OmniHeart provided food to participants, thus maximizing people’s ability to come as close as possible to the goals for each diet.
- All three diets tested provided the same high levels of potassium, magnesium, calcium and dietary fiber. And the diets were consistent in sodium and saturated fat content.
Three Variations Tested

Like OmniHeart variations, different kinds of dogs each have different strengths and fit different owners.
◊ Higher-Carbohydrate: closest to the original DASH diet, just slightly higher in carbohydrate due to more grains, fruit and added sugars compared to the original DASH pattern.
◊ Higher-Protein: replaced some of the carbohydrate in the original DASH diet with more protein. Some of that came from an increase in poultry, fish, lean meat and lowfat dairy. But most of the added protein came from increased use of legumes and nuts.
◊ Higher-Unsaturated Fat: reduced carbohydrate to the same level as in the higher-protein pattern, but did so by replacing some of the fruits and grains with extra monounsaturated and polyunsaturated oils.
How OmniHeart Variations of a DASH Diet Cut Cardiovascular Risk Factors
Blood Pressure: All three diets reduced systolic and diastolic blood pressure compared to people’s starting point; these changes were statistically significant and clinically meaningful. The diets higher in protein and in unsaturated fat reduced blood pressure slightly more, by about 9/5 mm Hg.
- In people who began with established hypertension, blood pressure dropped about 16/8 mm Hg with the protein and unsaturated fat diets.
LDL cholesterol: All three diets reduced LDL by over 11 mg/dL compared to baseline. However, only the higher-protein diet’s reduction was statistically significant (14.2 mg/dl).
- Among people whose LDL was initially over 130 mg/dL, LDL dropped an average of at least 20 mg/dL in six weeks on all three diets. (Note: these people were not taking any lipid-lowering medications.)
Triglycerides: The higher-carbohydrate diet did not change levels from baseline. Both the higher-unsaturated fat and higher-protein diets significantly reduced levels (by 9.3 and 16.4 mg/dl, respectively).
Insulin sensitivity: None of the participants in the OmniHeart study had diabetes. However, follow-up analysis showed that the diet higher in fat, which replaced some carbohydrate with unsaturated fat, improved two different measures of insulin sensitivity.
- In this study, improved insulin sensitivity with the diet higher in unsaturated fat occurred primarily in people who did not have overweight or obesity. So a higher-fat, lower-carbohydrate diet may help, but may not be as powerful in improving insulin function as an appropriate calorie level and modest weight loss, according to the study authors.
Inflammation (measured by hs-CRP blood levels): reduced by all three OmniHeart diets, with no difference between the diets.
Subclinical heart muscle damage (measured with the biomarker high-sensitivity cardiac troponin I) was decreased by each of the three diet variations compared to baseline diet. Changes were statistically significant, with no difference between the OmniHeart diets.
What Are the Basics of a DASH Diet?

Observational cohort studies use scoring systems to identify how dietary patterns are associated with health. Several different scoring systems have been created, and each translates the DASH principles into quantifiable points slightly differently.
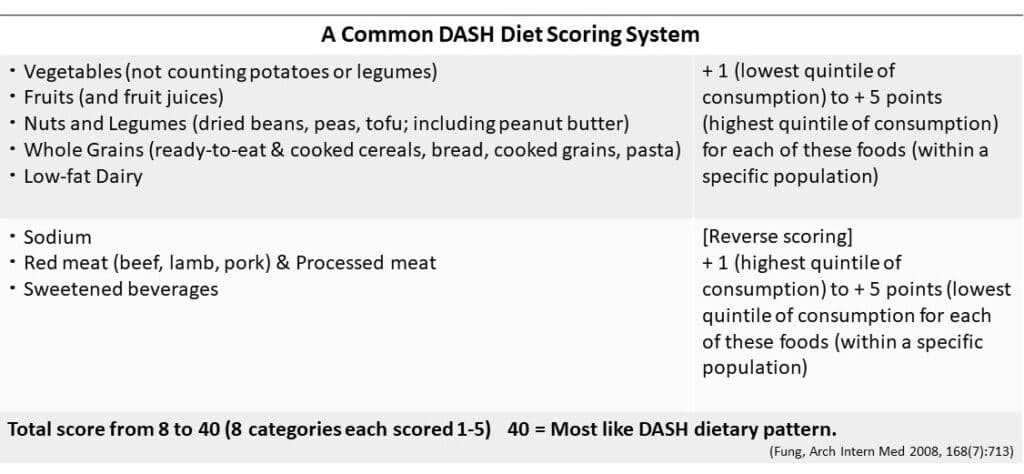
This DASH diet scoring system is among the most commonly used in observational population studies in the U.S. (for example, the Nurses’ Health Study prospective cohort study).
You can see that although fat content is not part of this scoring system, because of which food choices earn the most points, a high DASH diet score does represent a diet likely to be relatively low in saturated fat. Some other DASH scores include limits on fat consumption.
The consistent dietary pattern that DASH diet scores represent is a plant-forward pattern that includes low-fat dairy products and limits sodium, saturated fat, and added sugars. Share on X
What’s Easily Overlooked About a DASH Diet

Confused by the different variations on a DASH diet in the research? You’re not alone.
- It’s not simply low-sodium or high in vegetables and fruits. Limiting sodium is an important element of DASH, but the major outcome of those original DASH trials was that blood pressure drops most when combining increased vegetables and fruits and reduced sodium with lowfat dairy products and reduced saturated fat and sweets. It’s about limiting foods that increase cardiovascular risk and boosting foods with cardioprotective potential.
- It’s plant-focused, but not vegetarian. The clinical trials and scores used in population research on a DASH diet allow for modest consumption of lean meat, poultry, fish and dairy. For those who prefer, a DASH diet can meet core criteria without meat or poultry, including more legumes and increased fish is also an option. The diet was designed to include dairy products and provide 1200 mg/day of calcium — because overall research shows that calcium may help reduce blood pressure. It’s reasonable to substitute a plant-based dairy alternative that’s fortified with calcium for those who don’t want to include dairy products, although DASH diet research does not currently provide evidence on results of such a swap.
- What about dairy choices? In the randomized controlled trials, 75% of the dairy products were low-fat, which helped limit saturated fat content. That does allow for limited use of higher-fat dairy choices. For example, some may choose regular cheese, but low-fat or non-fat milk and yogurt. For people who don’t include regular (animal-based) dairy products, it’s more consistent with findings of overall cardiovascular research to reach the DASH diet’s 1000 to 1200 mg of calcium with food choices and avoid pushing calcium to extremes with high-dose supplements.
- What about alcohol? Alcohol is not assessed by any of the DASH diet scoring systems. However, controlled trials of the DASH diet always included instructions to limit alcohol to no more than two standard drinks per day.
- Compared to what? Studies that show a DASH diet to be a healthier dietary pattern often compare it to a typical American diet or to a low-fat diet that does not specify choosing nutrient-rich foods to replace high-fat foods. These studies can’t be interpreted to mean that DASH is more healthful than all other diets.
A Mediterranean DASH Diet? How to Create YOUR Best Plant-Based Diet

Just as choosing a paint color isn’t as simple as “blue” or “green”, you can blend features of a Mediterranean diet and a DASH diet for a healthy diet that works for you.
You can develop all kinds of variations on the traditional Mediterranean diet and basic DASH formula.
Individualization allows you to create an eating pattern that best meets individual needs and addresses important risk factors, as well as fitting with personal and family food preferences.
- The NU-AGE study (New Dietary Strategies Addressing the Specific Needs of Elderly Population for Healthy Aging in Europe) was a 1-year randomized controlled trial that adapted a Mediterranean diet by limiting sodium to 2000 mg/day and increasing low-fat dairy to 3 servings/day. After one year, compared to a control group continuing usual habits, those who changed their diet achieved clinically relevant reductions in blood pressure and arterial stiffness.
- The Blue Zones include five places around the world where people commonly not only live – but thrive — into their 100s. These countries represent vastly different cultures, specific native foods, and food flavoring traditions. Yet the overall dietary pattern is remarkably similar in embracing an abundance of vegetables, fruits, whole grains and legumes (whether dried beans, lentils, or soy foods).
- Want to learn more about Blue Zones? Check out my interview with Dan Buettner, author of several books about these areas and their healthy lifestyles.
- Okinawa, Japan, is one of the Blue Zones. For generations, people there have intoned the phrase “hara hachi bu” before each meal. It’s a reminder to stop eating when they’re 80% full. This technique can surprise you with how satisfied you are when you stop eating sooner than usual. And if you are satisfied with only 80% of your usual food, that accomplishes a calorie cut without counting or measuring… and without going hungry. That’s a technique that could be added to any of these Mediterranean or DASH diet options.
DASH Diet vs Mediterranean Diet: How to Gain the Most Value
Rather than getting distracted by their differences, start by focusing on what the Mediterranean diet, the DASH diet, and all three DASH OmniHeart variations have in common.
(1) Compared to typical U.S. eating habits, they all include MORE:
- Vegetables (including more dark leafy greens that supply so many protective nutrients and compounds)
- Fruits
- Whole grains
- Nuts and seeds
- Legumes (start with pulses (like dried beans and lentils) and soy foods at least three times a week, and work toward more)
- Unsaturated oils
(2) Compared to typical U.S. eating habits, they all include LESS:
- Sweet snacks and desserts
- Sugar-sweetened beverages
- Processed meats
- Highly-processed “snack foods”
(3) Personalize: Mediterranean-style diet, DASH diet and its OmniHeart variations all offer potential for improving heart health and reducing cancer risk.
You can’t compare results from different studies – involving completely different people – to identify a diet that’s “best”.
But the big picture from overall research does provide some suggestions:
- For those with (or at risk of) high blood pressure: make sure to limit high-sodium processed foods. Including enough calcium-rich foods may also help. And for those with overweight or obesity, following the example of the ENCORE study to modestly reduce calories and increase physical activity holds special value.
- With elevated LDL cholesterol, reducing saturated fat is important. Just be sure that it’s accomplished without increasing sweets and refined grains. Instead, look to dietary patterns that focus on more plant protein and unsaturated fat.
- With elevated triglycerides, prediabetes, or insulin resistance, steer towards the examples of a Mediterranean diet or the OmniHeart version of DASH higher in unsaturated fat. If you also have overweight or obesity, all these risk factors tend to improve by shaving off a few calories with vegetables occupying a greater proportion of your plate or more attention to hunger signals as a guide to eating.

Maybe not the “best” dog, but Lucky was the blend that was a perfect choice for us.
Whether you’re considering choices for eating habits, paint colors, or dogs, you’ve got lots of options… including a blend. We found a blend at our local Humane Society who was the best dog for me and my family, and we never looked back.
Bottom Line on a DASH Diet vs Mediterranean Diet
A DASH diet and Mediterranean diet are both plant-forward dietary patterns that promote heart health and fit recommendations for a diet to reduce cancer risk. Either one is far more healthful than typical American eating habits. Start with the common elements these dietary patterns share. Then individualize choices — creating a unique blend — to best fit individual health conditions and risk factors, personal and cultural food preferences, and what is or can be accessible.
Sign up: If you aren’t already receiving my research reviews by email, sign up so you won’t miss any of the fascinating topics coming in future reviews! Just click here.
Experiment with Different Ways to Make Healthy Eating Doable
• Whether Mediterranean or not, make healthy cuisine flavorful with garlic and onion, herbs, spices, splashes of vinegar or citrus….This is how you make healthy eating a delicious fit for YOU.
• Choose olive oil for an easy homemade salad dressing and on vegetables. Select extra-virgin olive oil if possible, since it contains plant compounds that may provide part of the protection, as reviewed here. Other oils, such as canola oil, can be smart choices, too.
• Step beyond deep-fried or as breaded fish. Get tips and try new ways to include fish and seafood at least two times a week (from the Seafood Nutrition Partnership).
For a baseline plan to reduce cancer risk that can incorporate a DASH diet or Mediterranean diet: the New American Plate from the American Institute for Cancer Research (AICR).
Learn more about the DASH diet
- Details about the diet and tips for success from the National Institutes of Health
- A free client-ready DASH diet handout from the National Lipid Association
- DASH Diet for Dummies (2nd edition, 2020): a book with information and recipes by Sarah Samaan, MD; Rosanne Rust, MS, RDN; and Cindy Kleckner, RDN, LD, FAND
Learn more about the Mediterranean diet
- A Mediterranean Diet Pyramid (& free materials) by Oldways
- A free client-ready Mediterranean diet handout from the National Lipid Association (and a version in Spanish)
Learn more about Blue Zones
- At the Blue Zones website
- From a pair of interviews I did with Dan Buettner starting here and then here.
Appel LJ, Moore TJ, Obarzanek E, et al. A clinical trial of the effects of dietary patterns on blood pressure. DASH Collaborative Research Group. N Engl J Med. 1997;336(16):1117-1124.
Appel LJ, Sacks FM, Carey VJ, et al. Effects of protein, monounsaturated fat, and carbohydrate intake on blood pressure and serum lipids: results of the OmniHeart randomized trial. JAMA. 2005;294(19):2455-2464.
Blumenthal JA, Babyak MA, Hinderliter A, et al. Effects of the DASH diet alone and in combination with exercise and weight loss on blood pressure and cardiovascular biomarkers in men and women with high blood pressure: the ENCORE study. Arch Intern Med. 2010;170(2):126-135.
Blumenthal JA, Babyak MA, Sherwood A, et al. Effects of the dietary approaches to stop hypertension diet alone and in combination with exercise and caloric restriction on insulin sensitivity and lipids. Hypertension. 2010;55(5):1199-1205.
Buettner D, Skemp S. Blue Zones: Lessons From the World’s Longest Lived. American Journal of Lifestyle Medicine. 2016;10(5):318-321.
Chiavaroli L, Viguiliouk E, Nishi SK, et al. DASH Dietary Pattern and Cardiometabolic Outcomes: An Umbrella Review of Systematic Reviews and Meta-Analyses. Nutrients. 2019;11(2).
Dinu M, Pagliai G, Casini A, Sofi F. Mediterranean diet and multiple health outcomes: an umbrella review of meta-analyses of observational studies and randomised trials. Eur J Clin Nutr. 2018;72(1):30-43.
Fu J, Liu Y, Zhang L, et al. Nonpharmacologic Interventions for Reducing Blood Pressure in Adults With Prehypertension to Established Hypertension. J Am Heart Assoc. 2020;9(19):e016804.
Gadgil MD, Appel LJ, Yeung E, Anderson CA, Sacks FM, Miller ER, 3rd. The effects of carbohydrate, unsaturated fat, and protein intake on measures of insulin sensitivity: results from the OmniHeart trial. Diabetes Care. 2013;36(5):1132-1137.
Jenkins DJA, Spence JD, Giovannucci EL, et al. Supplemental Vitamins and Minerals for Cardiovascular Disease Prevention and Treatment: JACC Focus Seminar. J Am Coll Cardiol. 2021;77(4):423-436.
Jennings A, Berendsen AM, Groot LCPGMd, et al. Mediterranean-Style Diet Improves Systolic Blood Pressure and Arterial Stiffness in Older Adults. Hypertension. 2019;73(3):578-586.
Juraschek SP, Kovell LC, Appel LJ, et al. Associations Between Dietary Patterns and Subclinical Cardiac Injury: An Observational Analysis From the DASH Trial. Ann Intern Med. 2020;172(12):786-794.
Juraschek SP, Kovell LC, Appel LJ, et al. Effects of Diet and Sodium Reduction on Cardiac Injury, Strain, and Inflammation. J Am Coll Cardiol. 2021;77(21):2625-2634.
Kovell LC, Yeung EH, Miller ER, 3rd, et al. Healthy diet reduces markers of cardiac injury and inflammation regardless of macronutrients: Results from the OmniHeart trial. Int J Cardiol. 2020;299:282-288.
Martínez-González MA, Gea A, Ruiz-Canela M. The Mediterranean Diet and Cardiovascular Health. Circulation Research. 2019;124(5):779-798.
Martínez-González MÁ, Hershey MS, Zazpe I, Trichopoulou A. Transferability of the Mediterranean Diet to Non-Mediterranean Countries. What Is and What Is Not the Mediterranean Diet. Nutrients. 2017;9(11):1226.
Morze J, Danielewicz A, Hoffmann G, Schwingshackl L. Diet Quality as Assessed by the Healthy Eating Index, Alternate Healthy Eating Index, Dietary Approaches to Stop Hypertension Score, and Health Outcomes: A Second Update of a Systematic Review and Meta-Analysis of Cohort Studies. J Acad Nutr Diet. 2020;120(12):1998-2031.e1915.
Morze J, Danielewicz A, Przybyłowicz K, Zeng H, Hoffmann G, Schwingshackl L. An updated systematic review and meta-analysis on adherence to Mediterranean diet and risk of cancer. Eur J Nutr. 2021;60(3):1561-1586.
Sacks FM, Svetkey LP, Vollmer WM, et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med. 2001;344(1):3-10.
Schwingshackl L, Chaimani A, Schwedhelm C, et al. Comparative effects of different dietary approaches on blood pressure in hypertensive and pre-hypertensive patients: A systematic review and network meta-analysis. Crit Rev Food Sci Nutr. 2019;59(16):2674-2687.
Shikany JM, Safford MM, Bryan J, et al. Dietary Patterns and Mediterranean Diet Score and Hazard of Recurrent Coronary Heart Disease Events and All-Cause Mortality in the REGARDS Study. J Am Heart Assoc. 2018;7(14).
Soltani S, Shirani F, Chitsazi MJ, Salehi-Abargouei A. The effect of dietary approaches to stop hypertension (DASH) diet on weight and body composition in adults: a systematic review and meta-analysis of randomized controlled clinical trials. Obesity Reviews. 2016;17(5):442-454.
Swain JF, McCarron PB, Hamilton EF, Sacks FM, Appel LJ. Characteristics of the diet patterns tested in the optimal macronutrient intake trial to prevent heart disease (OmniHeart): options for a heart-healthy diet. J Am Diet Assoc. 2008;108(2):257-265.
Tankeu AT, Ndip Agbor V, Noubiap JJ. Calcium supplementation and cardiovascular risk: A rising concern. J Clin Hypertens (Greenwich). 2017;19(6):640-646.
Trichopoulou A, Costacou T, Bamia C, Trichopoulos D. Adherence to a Mediterranean diet and survival in a Greek population. N Engl J Med. 2003;348(26):2599-2608.
Trichopoulou A, Martínez-González MA, Tong TYN, et al. Definitions and potential health benefits of the Mediterranean diet: views from experts around the world. BMC Med. 2014;12(1):112.
Villa-Etchegoyen C, Lombarte M, Matamoros N, Belizán JM, Cormick G. Mechanisms Involved in the Relationship between Low Calcium Intake and High Blood Pressure. Nutrients. 2019;11(5):1112.
World Cancer Research Fund/American Institute for Cancer Research. Diet, Nutrition, Physical Activity and Cancer: a Global Perspective. Continuous Update Project Expert Report 2018. Available at dietandcancerreport.org.
Door choices: Letizia Bordoni on Unsplash.com
Mediterranean diet photo: bialasiewicz at 123rf.com – 68548803
Dog reading about a Mediterranean diet: 2Photo Pots on Unsplash.com
Dog confused about a DASH diet: Dex Ezekiel on Unsplash.com
Paint color choices: Clay Banks on Unsplash.com
4 Comments
Leave a Comment
Published : August 31, 2021 | Last Updated: June 12, 2023
Tagged: Anti-Inflammatory Diet, DASH diet, healthy diet, healthy eating, heart disease, heart health, high blood pressure, hypertension, Med diet, Mediterranean DASH diet, Mediterranean diet, nuts, plant-based diet, reducing cancer risk, vegetables
Meet the author/educator
I Take Nutrition Science From Daunting to Doable.™
As a registered dietitian nutritionist, one of the most frequent complaints I hear from people — including health professionals — is that they are overwhelmed by the volume of sometimes-conflicting nutrition information.
I believe that when you turn nutrition from daunting to doable, you can transform people's lives.
Accurately translating nutrition science takes training, time and practice. Dietitians have the essential training and knowledge, but there’s only so much time in a day. I delight in helping them conquer “nutrition overwhelm” so they can feel capable and confident as they help others thrive.
I'm a speaker, writer, and nutrition consultant ... and I welcome you to share or comment on posts as part of this community!




Really well written and thorough review. Thanks — such nice work, and very helpful.
Thank you for the positive feedback, Dr. Doan. I’m so glad that distilling and summarizing the information on these 2 popular (and effective) dietary patterns can help you give sound advice to your patients. Keep in touch!
Karen, what a wonderful review of DASH,Mediterranean Diets and all the variations. Very thorough and well summarized. I also love the dog analogy of which is best? It depends!
I’m so glad you found this research review — and the dog analogy — helpful, Bridget. I do think the “best dog” quest is a good parallel for the multiple different choices available for a diet that supports health. How much better to get going creating one that works for each individual than to dither back and forth about which one is perfect!